A coeliac disease test in NZ typically begins with a specific blood screening called tTG-IgA to detect antibodies. If positive, a gastroscopy with a small bowel biopsy is required to confirm the diagnosis. Crucially, you must continue eating gluten daily for at least six weeks prior to testing to ensure accurate results.
Navigating the medical system to get a confirmed diagnosis for coeliac disease can be confusing and stressful. In New Zealand, the process follows a strict clinical pathway designed to ensure accuracy and prevent misdiagnosis. Whether you are experiencing chronic fatigue, gastrointestinal distress, or iron deficiency, understanding the specific diagnostic steps required by Te Whatu Ora (Health New Zealand) and private specialists is essential for your long-term health.
Why Must You Keep Eating Gluten Before Testing?
The most critical error patients make when seeking a coeliac disease test in NZ is removing gluten from their diet too early. It is common for individuals to feel unwell, suspect gluten is the cause, and immediately stop eating bread and pasta. However, doing so can render your medical tests useless.
Coeliac disease is an autoimmune condition where the body attacks its own tissues in response to gluten. If you remove the trigger (gluten), the immune response calms down, antibody levels in the blood drop, and the gut lining begins to heal. Consequently, a test performed on a gluten-free diet may return a “false negative,” leaving you without a diagnosis and potentially causing future health complications.

How much gluten is required for a valid test?
According to Coeliac New Zealand and international guidelines, you must undertake a “gluten challenge” if you have already removed gluten from your diet. The general recommendation for adults is to consume the equivalent of four slices of wheat-based bread per day for at least six weeks prior to both blood tests and biopsies.
This period can be physically difficult for those with active disease. If your symptoms are severe, consult your GP or gastroenterologist. In some cases, they may shorten the duration to two weeks for the biopsy, but the six-week mark remains the gold standard for serology (blood tests).
What Blood Tests are Used for Coeliac Disease?
The first step in the diagnosis process is serology. Your General Practitioner (GP) will request a specific panel of blood tests. It is not enough to simply ask for a “gluten test”; the lab needs to look for specific autoimmune markers.
Understanding tTG-IgA Levels
The primary screening test used in New Zealand is the Tissue Transglutaminase IgA (tTG-IgA) test. Tissue transglutaminase is an enzyme in the intestine. In people with coeliac disease, the body produces antibodies against this enzyme when gluten is present.
- Negative Result: Usually indicates coeliac disease is unlikely, provided you have been eating gluten and do not have an IgA deficiency.
- Weak Positive: Suggests a possibility of coeliac disease; further investigation is needed.
- Strong Positive: Highly indicative of coeliac disease, making a biopsy necessary for confirmation.
The Importance of Total IgA
Alongside the tTG-IgA, your doctor should request a Total IgA count. Approximately 2-3% of people with coeliac disease have a condition called IgA deficiency. If you are IgA deficient, the standard tTG-IgA test will produce a false negative, regardless of whether you have coeliac disease. If a deficiency is found, the lab will run a Deamidated Gliadin Peptide (DGP-IgG) test instead.
What to Expect During an Endoscopy?
While blood tests are excellent screening tools, the gastroscopy (endoscopy) with duodenal biopsy remains the gold standard for diagnosis in New Zealand adults. This procedure allows a gastroenterologist to visually inspect the small intestine and take tiny tissue samples to check for damage to the villi.
The Procedure: Sedation vs. Throat Spray
In New Zealand, you are typically offered a choice between a throat spray (local anaesthetic) and intravenous sedation.
- Throat Spray: Numbs the back of the throat to suppress the gag reflex. You remain fully awake and aware. The benefit is a faster recovery time; you can often drive yourself home shortly after.
- Sedation: This is not a general anaesthetic; you are technically awake but in a “twilight” state. Most patients feel very relaxed and often do not remember the procedure. You will need someone to drive you home and stay with you for 24 hours.
During the procedure, a thin, flexible tube with a camera is passed down the oesophagus, through the stomach, and into the small intestine. The specialist will take several biopsies (usually 4-6) from different parts of the duodenum, as the damage caused by coeliac disease can be patchy.
Public vs Private Health System Wait Times
One of the biggest challenges for Kiwi patients is the disparity between the public and private health systems. Once your GP has a positive blood test result, they will refer you to a gastroenterologist.
Public System (Te Whatu Ora)
In the public system, referrals are triaged based on severity and available resources.
- Cost: Free for NZ residents and citizens.
- Wait Times: These vary significantly by region. In major centres like Auckland or Christchurch, wait times for a non-urgent gastroscopy can range from 4 to 12 months. During this wait, you are generally expected to continue eating gluten to maintain the validity of the biopsy, which can be difficult for symptomatic patients.
Private Sector
If you have medical insurance or are self-funding, you can see a private specialist.
- Cost: A consultation and gastroscopy package can range from $1,500 to $2,500 NZD if self-funding.
- Wait Times: typically much shorter, often ranging from 2 to 6 weeks. This significantly reduces the duration you need to maintain a gluten-containing diet while feeling unwell.

The Role of Genetic Testing
Genetic testing is not a standalone diagnostic tool for active disease, but it plays a specific role in the coeliac disease test NZ landscape. The test looks for Human Leukocyte Antigen (HLA) markers, specifically HLA-DQ2 and HLA-DQ8.
When is genetic testing useful?
Over 99% of people with coeliac disease carry one or both of these genes. However, approximately 30-40% of the general population also carries them but never develops the disease. Therefore:
- A Positive Genetic Test: Does NOT mean you have coeliac disease. It only means you have the genetic susceptibility.
- A Negative Genetic Test: Effectively rules out coeliac disease for life.
Genetic testing is particularly useful for patients who have already gone gluten-free and refuse to do a gluten challenge. A negative gene test can save them from an unnecessary gluten challenge. This test can be ordered by a GP or purchased privately, though it is expensive and not always funded in the public system.
Interpreting Biopsy Results: The Marsh Scale
Once your biopsy is complete, the tissue samples are sent to a pathologist for analysis. They use a classification system called the Marsh Scale (or Modified Marsh Classification) to grade the severity of the damage to the intestinal villi.
- Marsh 0: Normal mucosa. No coeliac disease.
- Marsh 1: Increased number of intraepithelial lymphocytes (white blood cells) but normal villi structure. This is non-specific and can be caused by other things, though it may be early coeliac disease.
- Marsh 2: Increased lymphocytes and crypt hyperplasia (deepening of the grooves between villi).
- Marsh 3 (a, b, c): This indicates villous atrophy. The villi are flattened or completely destroyed. Marsh 3 is the definitive confirmation of coeliac disease.
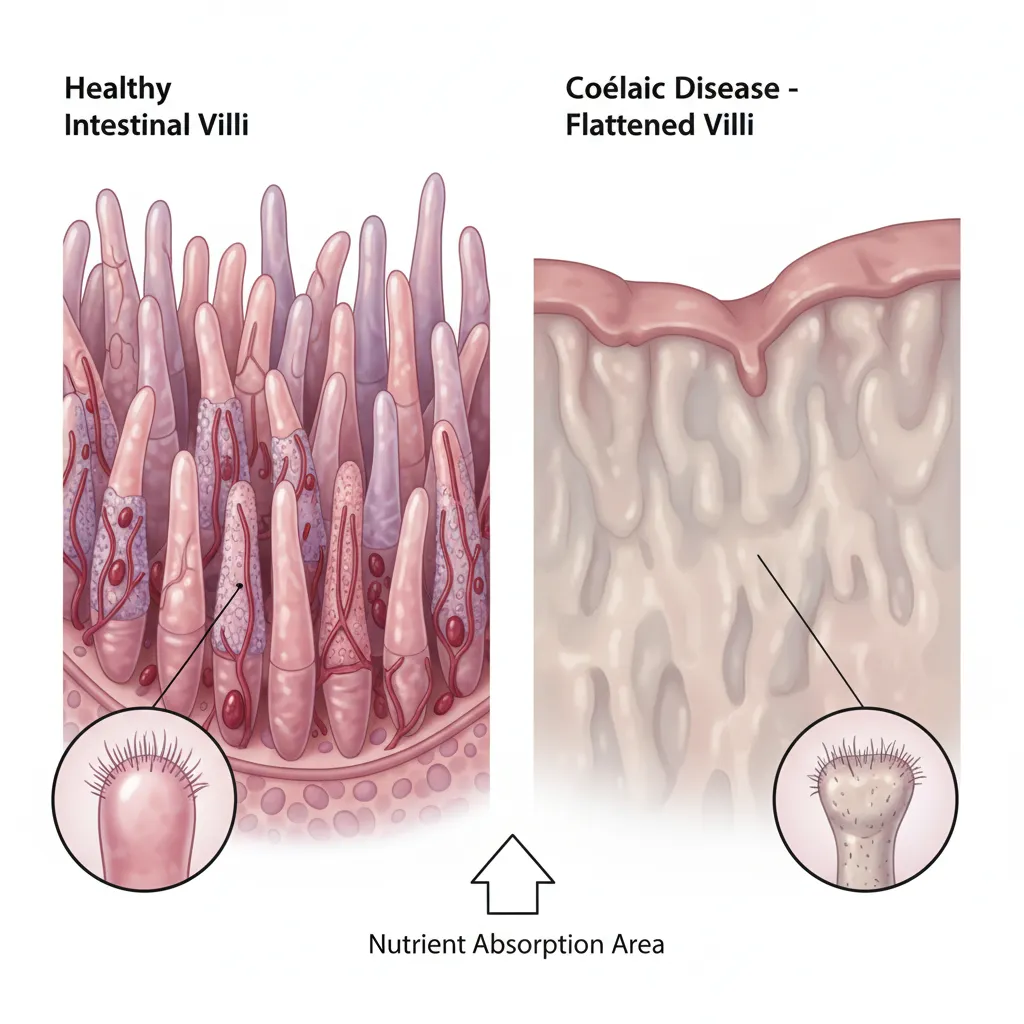
Upon receiving a Marsh 3 diagnosis, your doctor will officially diagnose you with coeliac disease. At this point, you will be instructed to begin a strict, lifelong gluten-free diet. In New Zealand, a confirmed diagnosis also allows you to access the Disability Allowance (subject to income testing) to help offset the higher cost of gluten-free food.
Summary of the NZ Diagnosis Pathway
To summarize, the journey to a diagnosis involves:
- Symptoms appear: Do not stop eating gluten.
- GP Visit: Request tTG-IgA and Total IgA blood tests.
- Referral: If bloods are positive, get referred to a gastroenterologist (Public or Private).
- Gluten Challenge: Continue eating gluten until the procedure.
- Gastroscopy: Biopsies are taken from the small bowel.
- Histology: Pathologist confirms villous atrophy (Marsh 3).
- Diagnosis: Begin gluten-free life and join Coeliac New Zealand for support.
People Also Ask
Can I get tested for coeliac disease at a pharmacy in NZ?
Some pharmacies in New Zealand sell self-test kits that detect antibodies from a finger-prick blood sample. However, these are screening tools only and are not sufficient for a medical diagnosis. A positive result from a pharmacy kit must always be followed up with a formal venous blood test and a biopsy ordered by a doctor.
How much does a coeliac test cost in NZ?
In the public system, blood tests and biopsies are free for eligible residents. In the private sector, a GP consultation is roughly $50-$100, blood tests may cost roughly $100 if not funded, and a private endoscopy typically costs between $1,500 and $2,500.
Can children be diagnosed without an endoscopy in NZ?
Yes, under strict criteria. The European Society for Paediatric Gastroenterology Hepatology and Nutrition (ESPGHAN) guidelines, adopted in NZ, allow for a non-biopsy diagnosis in children if tTG-IgA levels are very high (10x the upper limit of normal) and a second blood sample confirms positivity, usually alongside positive genetic testing.
What happens if my blood test is negative but I still feel sick?
If your coeliac screen is negative but symptoms persist, you may have Non-Coeliac Gluten Sensitivity (NCGS), IBS, or another gastrointestinal issue. It is important to rule out coeliac disease first before experimenting with elimination diets under the guidance of a dietitian.
How long does it take to get biopsy results in NZ?
After your endoscopy, the tissue samples are sent to a laboratory. In the private sector, results are typically available within 3 to 7 days. In the public system, it may take slightly longer, usually between 1 to 2 weeks, before your GP or specialist contacts you with the findings.
Is coeliac disease covered by medical insurance in NZ?
Yes, most comprehensive medical insurance policies in New Zealand cover the diagnostic process (specialist consultations and gastroscopy) if the condition was not a pre-existing condition when you took out the policy. Check your specific policy wording regarding diagnostic procedures.
